
America's
Seniors & Their Families Make Informed Decisions About
Medicare With Best Medicare Supplement .com
We
are pleased to provide you with a copy of the our Guide to Medicare Supplement Insurance. This
guide includes many tips on choosing a Medicare supplement. Federal
and state regulations require insurance companies to provide Medicare
supplement policies that are limited to no more than 14 standard
benefit plans. Each of the 14 plans must cover specific expenses.
This guide will make it easier for you to compare plans and
premiums.
In 2012, Medicare has made some major changes including the introduction
of Medicare Part D. If you currently have a Medicare Supplement
Plan M and N please discuss your options with your local agent
or with our knowledgeable customer care representative. As you use
this guide, please keep in mind that it is just that, a guide, to
assist you with your purchasing decision. Shop carefully, take your
time and contact us if you have questions. Our staff has extremely
knowledgeable staff members who are dedicated to assisting you with
a wide range of insurance questions or problems.
All the plans MUST include the following basic benefits:
- Hospital coinsurance coverage
- 365 days of full hospital coverage
- Reimbursement for the 20% of the cost of your medical care that Medicare does not cover.
- The first 3 pints of blood you need each year.
Depending on which Medicare Insurance plan you choose, you can get extra coverage for the expenses that Medicare doesn’t cover, such as:
- Hospital deductible
- Skilled nursing facility coinsurance
- Emergency care outside the U.S.
- At home recovery care
- Part B excess charges
- Preventative care
- Prescription drug coverage with Medicare Part D
Return to Top
Medicare is the federal government program that gives you health care
coverage if you are age 65 or older, or have a disability, and are
a US citizen or have been a permanent legal resident for at least
5 continuous years, regardless of your income. Medicare Suppelement Insurance is divided
into a number of parts.
Medicare Part A covers inpatient
hospital, skilled nursing facility, home health care and hospice care.
Medicare Part B covers almost
all reasonable and necessary Medicare Medical services, including doctors’
services, laboratory and x-ray services, durable medical equipment
(wheelchairs, hospital beds etc.), ambulance services, outpatient
hospital care, home health care, blood and medical supplies.
Medicare Part C is called “Medicare
Advantage” and is an optional plan that will combine all the
benefits of Medicare Parts A & B, as well as Medicare prescription drug coverages and may provide some or all of the benefits previously available
through a standardized Medicare supplement plan. These Medicare Advantage
Plans may be “Managed Care” type plans such as HMO, PPO,
or Private Fee for Service plans.
Medicare Part D is the optional Medicare prescription drug coverage and makes coverage for prescription
drugs available to all people with Medicare.
What is a benefit period?
A benefit period begins on the first day of a Medicare-covered inpatient
stay. It ends when you have been out of the hospital or skilled nursing
facility for 60 consecutive days. A new benefit period begins and
the beneficiary must pay a new inpatient hospital deductible. There
may be as many as five Medicare benefit periods in a calendar year.
Will
Medicare cover all medical expenses?
No. Medicare only covers a portion of health care costs. A Medicare
supplement helps with expenses not fully paid by Medicare.
Do supplements cover all charges Medicare doesn’t?
No. Supplements will not cover expenses if Medicare doesn’t
pay a portion of the bill, with some exceptions.
What if Medicare considers a service to be unnecessary?
If physicians recommend a procedure that they are (or should be) aware
is not covered by Medicare, they are required to notify you in writing
that Medicare will not provide Medicare coverage for the service. Similarly, if a surgeon
does not accept assignment for elective surgery, the physician must
give you a written estimate if the charge will exceed $500.
What is assignment?
It is the acceptance of the charges allowed by Medicare as payment
in full.
What is limiting charge?
Physicians who do not accept assignment are limited to charging 115
percent of the fee schedule for nonparticipating doctors.
What is issue age?
The premium is established when you buy your policy. You continue
to pay the premium required of a person who is the same age you were
when you bought your policy. For example, if you buy a policy at age
65, you always will pay the rate that the company charges people who
are 65, regardless of your age.
What is the attained age?
The premium is based on your current age and increases automatically
as you grow older. Typically, these plans are less expensive for younger
individuals, but may cost considerably more in later years.
Can I be eligible if I’m under 65?
A person can qualify for Medicare under age 65 if they meet certain
criteria for disability. If you receive continuing dialysis for permanent
kidney failure or need a kidney transplant you could be eligible for
Medicare. If you are disabled and have been receiving Social Security
Disability payments for at least 2 years or if you have Amyotrophic
Lateral Sclerosis (ALS - Lou Gehrig’s disease) you could also
be eligible for Medicare.
How do I know how much coverage to buy?
It is important to know how to assess your need for insurance in every
type of coverage you buy. With a Medicare supplement comparison, you should
review your medical care costs for the preceding year, assess your
current health status and choose a plan that is affordable. You may
want to consider enrolling in a Medicare Part D plan if you currently
are taking medications. The cost of prescription drugs has increased
dramatically in the last few years.
Return to Top
The Qualified Medicare Beneficiary Program and Spousal Impoverishment
Program are available to assist seniors. These are important benefits
if you have limited income and assets or if your spouse is in a long-term
care facility.
 The
Qualified Medicare Beneficiary Program is designed to provide
Medicare premiums, deductibles and coinsurance for seniors with
limited incomes. The federal government sets the income level
for individuals and couples each year. To find out if your income
qualifies, contact the government welfare office in your county.
This program will not pay for expenses that Medicare does not
allow. The
Qualified Medicare Beneficiary Program is designed to provide
Medicare premiums, deductibles and coinsurance for seniors with
limited incomes. The federal government sets the income level
for individuals and couples each year. To find out if your income
qualifies, contact the government welfare office in your county.
This program will not pay for expenses that Medicare does not
allow.
You may
suspend your Medicare supplement policy upon enrollment in the Qualified
Medicare Beneficiary Program. You will need to notify your insurance
company in writing of your eligibility within 90 days. If you lose
your eligibility for the beneficiary program, you may reactivate your
Medicare supplement policy by notifying the insurer in writing and
paying the premium within 90 days of the termination of your eligibility.
The Specified
Low Income Beneficiaries Program assists individuals with slightly
more income than those who are Qualified Medicare Beneficiaries by
paying their Part B premiums each month. Individuals and couples with
monthly income in a range specified by the federal government qualify.
In addition to the income limit, financial resources including bank
accounts, stocks and bonds cannot exceed $4,000 for an individual
or $6,000 per couple (2006 numbers which rise with inflation).
Under the Spousal Impoverishment Program, when a spouse enters a long-term
care facility, there are rules for the division of the couple’s
assets. The spouse at home may retain a maximum of half the couple’s
resources, not to exceed a maximum set by the federal government.
Certain assets are exempt, including the home, household goods and
one car.
There are regulations concerning the amount of income the
spouse at home may retain on a monthly basis. Either spouse may request
an assessment of resources when one spouse enters a nursing home.
You will need to contact your county welfare office for more information.
Return to Top
Preventative Health Benefits
All newly enrolled Medicare beneficiaries will be covered for certain
potentially life saving preventative benefits. These benefits include
an initial preventative physical examination which includes baseline
measurement of height, weight and blood pressure, an electrocardiogram,
education counseling and referral related to other Medicare-covered
preventative services, such as vaccinations, screening mammography,
pap smears and pelvic exams and prostate and colon cancer screening
as well as blood tests required for cardiovascular screening, Glaucoma
screening and diabetes screening, medical nutritional therapy with
no deductible or co-pay.
Return to Top
Definition of Open Enrollment
Medicare Supplement companies that sell Medicare supplements are required to
issue policies to seniors who qualify for Medicare Part B because
they have reached age 65, without regard to their current health status.
This open enrollment period lasts six months beginning with eligibility
for Part B of Medicare.
 Companies may not refuse to issue a Medicare Supplemental Insurance to you or delay the issue of the policy based on your medical condition, health status, claims experience or receipt of health care.
The company may impose a six-month pre-existing condition clause during the first six months of the policy. If you delay enrollment in Part B of Medicare and are covered by a plan provided by your or your spouses employer, you will have an open enrollment period starting with the month in which you no longer are covered by your employer insurance. Companies may not refuse to issue a Medicare Supplemental Insurance to you or delay the issue of the policy based on your medical condition, health status, claims experience or receipt of health care.
The company may impose a six-month pre-existing condition clause during the first six months of the policy. If you delay enrollment in Part B of Medicare and are covered by a plan provided by your or your spouses employer, you will have an open enrollment period starting with the month in which you no longer are covered by your employer insurance.
Your open enrollment period will start when your Part B coverage becomes effective.
If you miss your open enrollment period, contact your local Social
Security Office. There may be that the initial open enrollment period
for Medicare Part D for all people with Medicare began already and
you do not have coverage for prescription drugs through a current
health plan such as aa person chooses to enroll in a Medicare Advantage
Plan for the first time and within the open enrollment plan.
Part
B Charges
There may be a waiting period for coverage and premium payments due.
Some individuals are eligible for Medicare due to a disability and
are under age 65. The open enrollment period applies to these individuals
upon turning 65.
Every year, if you wish, you may change your Part D plan between November
15th and December 31st. If you are just coming into the Medicare system,
you will have open enrollment for a period of twelve months.
Part D plan that coincides with the open enrollment period for Medicare
Part B. If you are coming from a retiree plan from a former employer
or a Medicare Advantage Plan with a drug benefit, you should consider
enrolling in Medicare Part D. If you do not have other credible drug
coverage and do not enroll in a Medicare Part D plan when you are
first eligible, you may be subject to substantial late enrollment
penalties. If first 12 months that person decides they no longer want
to be in that plan, they may, within withdraw.
During the first 12 months, return to “traditional” Medicare
and a Medicare Supplement policy without prejudice or the application
of elimination periods for pre-existing conditions.
Health
care providers are required to bill Medicare directly for beneficiaries.
Amounts billed on Part B of Medicare may not exceed 115 percent of
the Medicare allowable amount. The law requires physicians to refund
charges over 115 percent within 30 days.
Return to Top
Medicare Hospital Insurance – Medicare Part A (2012)
Medicare pays for all but $1,024.00 of your hospital stay during each
benefit period for reasonable and necessary care in the first 60 days
of confinement. For the next 30 days, it pays all but $256.00 a day
for covered services. Medicare pays expenses in excess of $512.00
a day during the 91st through 150th days. These are Lifetime Renewable
Days and may be used only once. If you are hospitalized more than
150 days, Medicare pays nothing.
A benefit period begins the first day of hospitalization and ends
when you have been out of a hospital or skilled nursing facility for
60 consecutive days. It is possible to have more than one benefit
period and more than one hospital deductible in a calendar year.
Charges for skilled nursing facility stays may be paid by Medicare
if the facility is a Medicare-certified facility. To qualify for this
benefit, you must have been hospitalized for at least three days and
have been admitted to the nursing facility within 30 days of discharge
from the hospital. The first 20 days are covered at 100 percent provided
you are receiving skilled care. The next 80 days Medicare pays amounts
more than $128.00 a day. Beyond the 100th day, Medicare pays nothing.
Under certain conditions, home health care is available for homebound
beneficiaries. This coverage includes skilled nursing services, occupational
therapy, and physical and speech therapy if provided by a Medicare-certified
home health service and if determined to be medically necessary. If
your physician establishes a care program that requires durable medical
equipment, Medicare will pay 80 percent of the Medicare-approved cost
of the equipment.
Medicare provides coverage for hospice care for patients certified
as terminally ill. This benefit is divided into two 90-day hospice
benefit periods and one 30-day benefit period. A subsequent extension
also may be covered. You pay for the first three pints of blood and
Medicare pays for any additional blood.
Medicare Medical Insurance - Medicare Part B (2012)
 Medicare covers physician services, outpatient hospital services,
lab services, X-ray, radiation and therapy services, home health visits,
physical therapy, speech pathology services, some forms of vaccinations,
durable medical equipment, limited ambulance services, prosthetic
devices, immunosuppressive drugs for the first year following an organ
transplant, and other medical supplies and equipment. Medicare covers physician services, outpatient hospital services,
lab services, X-ray, radiation and therapy services, home health visits,
physical therapy, speech pathology services, some forms of vaccinations,
durable medical equipment, limited ambulance services, prosthetic
devices, immunosuppressive drugs for the first year following an organ
transplant, and other medical supplies and equipment.
In 2012, the Part B premium is $96.40 a month. You are not required to purchase Part B, but it is an excellent buy because the federal government pays most of the actual cost. The Part B deductible is the first $135.00 of expenses in a calendar year. After the deductible, Medicare pays 80 percent of the approved charges. The Medicare deductible for blood expense is the cost of the first three pints.
Return to Top
Medicare Advantage Plan - Medicare Part C
Medicare Advantage Plans offer an alternative to “traditional”
Medicare plus a Medicare Supplement policy. Medicare Advantage plans will act as a single servicing point for Medicare for Medicare Parts
A & B billing functions. These plans can operate as PPO (preferred
provider organization), Managed Care Plan, HMO Plan, Private Fee for Service
plan, or as a Specialty plan as approved by Medicare.
Under a Managed
Care, PPO or HMO type plan, you may have to use doctors and hospitals
that are in that plan network or you may have to pay a larger co-pay
or other charges if you choose a medical provider that is not a member
of your plan. A company that offers Medicare Advantage plans may offer
coverage with a national, regional or local service area. Medicare
Advantage Plans may include a prescription drug plan equal to or better
than a standard Medicare Part D plan or they may require participants
to enroll in a separate Medicare Part D plan.
Return to Top
Medicare Prescription Drug Program - Medicare Part D
All people with Medicare are eligible to enroll in plans that cover
prescription drugs. The premium for this coverage will range from
less than $10 per month to about $99 per month and there may be an
annual deductible of up to $250. All plans must offer at least the
minimum standard benefits as set forth by Medicare but may offer significantly
more coverage.
The Medicare “standard” benefit states
– after your $250 deductible is met, you will pay 25% of your
prescription drug costs and Medicare will pay 75% until your total
prescription drug cost reach $2,250. You will then pay 100% of your
prescription drug costs until your total prescription drug costs reach
$5,100. After your total prescription drug costs reach $5,100 you
will pay a 5% co pay per prescription and Medicare will pay the remaining
95%.

The Medicare Prescription Drug benefit will include additional assistance for people with lower incomes. Most significantly, people with Medicare who are also eligible for Medicaid will receive full premium subsidy, full subsidy of the deductible and minimal co-pays, usually between $2-$5 per prescription.
Other people
with Medicare with lower incomes may receive premium and deductible
assistance and/or have limited co-pay from their Social Security.
Return to Top
New for 2006 – Medicare Supplement Plans K & L
Beginning in January of 2006, there will be 2 new Medicare Supplement
Plans available. These Plans will be titled K & L.
 Plan K: Plan K:
A person who chooses a Medicare Supplement Plan K will have a 50%
co-pay for Medicare eligible expenses including your Part A deductible,
skilled nursing co-insurance, your first three pints of blood, hospice
care, and Part B deductible until
such time as your “Out of Pocket” expenses reach $4,440
(for 2012). After a person reaches their out of pocket expense threshold,
Plan K will pay 100% of Medicare eligible expenses.
Plan L:
A person who chooses Medicare supplement plan L will have a 75% co-pay after their deductible is met until their Out of Pocket expenses reach the Plan L threshold of $2,220 (for 2012). After out of pocket threshold is reached, Plan L will pay 100% of Medicare eligible expenses.
The 75% co-pay applies to Medicare Part A & B deductibles as well as skilled nursing care co-insurance, your first 3 pints of blood and hospice care. Both Plans K & L include coverage for an additional 365 days of inpatient hospital care after other Medicare benefits are exhausted. The Out of Pocket thresholds for both plans K & L are indexed to inflation and may increase over time.
Return to Top
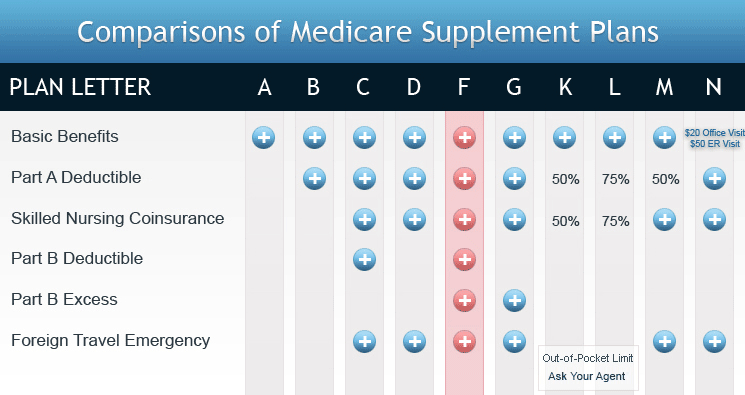
Compare Medicare Supplement Insurance Rates
Medicare cost-sharing out-of-pocket maximum (once met, plan pays 100%
all covered items) $4,440 and $2,220 core benefits pay the patient’s
share of Medicare’s approved amount for physician services 20%
after a $135 annual deductible, the patient’s cost of a long
hospital stay ($256/day for days 60-90, $512 for days 91-150, all
approved costs not paid by Medicare after day 150 to a total of 365
days lifetime) and charges for the first three pints of blood not
covered by Medicare.
Plans H, I and J with drug coverage included will not be availbe to new policyholders. These plans included prescription drug coverage in the past and will continue to be in force to existing policyholders. The new Plans H, I and J do not include prescription drug coverage. Of course, the Part D drug coverage can be purchased as a seperate policy.

Current policyholders may choose to remain in their existing plan H, I or J, or they may retain the plan without the drug benefit and enroll in Part D, or they may choose to change to a different Medicare supplement plan or enroll in a Medicare Advantage Plan.
*Plan F has options called high deductibles, which pay the same or
offer the same benefits as Plans F and J after the insured has paid
a calendar year ($1,900) deductible. Benefits from high deductible
Plan F will not begin until out-of-pocket expenses reach $1,900.
Out-of-pocket expenses for this deductible are expenses that ordinarily
would be paid by the policy.
These expenses include the Medicare deductibles
for Parts A and B, but do not include, in Plan J, the plan’s
separate prescription drug deductible or, in Plan F, the separate
foreign travel emergency deductible.
* Skilled Nursing Facility Coinsurance – For
Days 21-100.
Return to Top
1. Did
the agent try too hard to convince you of the possibility of you becoming
bankrupt, of your plans for retirement being disrupted, or of your
savings and that of your children or relative being wiped out because
of extended illness?
2. Did the Medicare supplement agent lead you to believe he or she was a representative
of the Medicare program, Insurance Department or other government
agency?
3. Did the agent suggest you drop a policy you already have in order
to buy the policy he or she was selling?
4. If you already have purchased a policy from an agent, has that
agent changed companies and suggested you change your policies over
to one offered by the agent’s new Medicare
supplement company?
5. Did the agent suggest you falsify any information on the policy?
6. Did the agent discourage you from shopping around or checking out
the policy thoroughly before deciding whether to buy it? Did he or
she make you feel like you had to sign up the same day?
7. Did the agent ask you to pay in cash or make your check out to
him or her personally or to the agency, instead of the company?
8. Did the agent fail to explain the policy to you or answer your
questions completely?
9. Did the agent complete your health history information on the application
exactly as you explained it before you signed the application?
10. Check with a reliable source if you have any questions about the
authenticity of any Medicare prescription drug card being offered
- before you buy!
Return to Top
Changes in federal law make it easy to shop for Medicare Supplement Insurance coverage. Before you start comparing policies, consider
these five suggestions:
1. Learn about Medicare’s
basic coverage and gaps.
2. Study the 14 standard Medicare Supplement Insurance plans. Decide
what coverage would best meet your health needs and financial circumstances.
3. Compare only the policies that meet your needs. Although the
benefits are identical for all Medicare Insurance plans
of the same type, premiums vary widely among companies and so does
the potential for premium increases.
4. Consider your alternatives. If you have limited income and assets,
you may qualify for free coverage through other government programs.
5. Contact your state health insurance counseling program for an
impartial, free review of your existing coverage.
Return to Top
The Medicare Supplement Insurance Guide tells us: Don't Be A Victim of Insurance Fraud
Often overlooked, insurance is one of the most costly bills we pay each
month. We encourage consumers to keep a watchful eye on your insurance
bills. Information is the key to avoiding insurance problems and scams.
Common Insurance Schemes:
- Overcharging for premiums.
- Collecting annual premiums but submitting only quarterly payments
to insurance companies.
- Not returning refunds from companies to the insured person.
To Avoid Becoming a
Victim
- Insist on delivery of documents within 30 days of the application.
- Call the company yourself to confirm coverage.
- Read the documents you receive and ask questions. Make agents and companies reply to inquiries in writing.
- Remember, Medicare Insurance will NEVER call or visit your home to solicit personal information such as such as your social security number or your credit card numbers.
Return to Top
The Medicare Supplement Guide's Definitions
In order to make a wise purchase, it is important to become familiar
with the terms used by Medicare and Medicare Insurance policies.
You may wish to familiarize yourself with the following terms:
ASSIGNMENT: The transfer by the policyholder of some or all
of his or her rights under a policy to another party. If assignment
is noted on the claim form, the insurance company will pay the health
care provider directly. Medicare assignment means the provider will
accept the Medicare-approved amounts for covered services as payment
in full. The beneficiary would then be responsible for any unmet deductible
applied to the charge, for the co-insurance and for any services that
were not approved.
COPAYMENT: Your portion or percentage of a health expense.
For example, the insurance would pay 80 cents of every dollar on the
provider’s charges. You pay the remaining 20 cents. With Medicare,
the coinsurance would be based on Medicare-allowable charges.
DEDUCTIBLE: The amount of covered expenses you must pay before
benefits become payable by the insurers.
EXCLUSIONS OR LIMITATIONS: Specified conditions, circumstances
or services not covered by the policy.
GUARANTEED RENEWABLE: The insurance company agrees to continue
insuring you so long as you pay the premium. The company reserves
the right to non-renew all contracts in the state.
MEDICARE-ALLOWABLE CHARGES: The amount deemed reasonable by
Medicare for a given medical service. Benefits are based on Medicare-allowable
charges, which may be less than the provider’s charges.
PRE-EXISTING CONDITIONS: A physical condition that existed before
the policy became effective. Federal law does not allow Medicare supplement
polices to exclude coverage for more than six months after the effective
date of the policy on the grounds that a condition existed prior to
the effective date of coverage.
Companies that replace a Medicare
supplement policy must waive the pre-existing waiting period on the
replacement policy. If the insured has not completed the waiting period
on the first policy, any period of time that was completed must be
credited on the new policy.
This does not apply to those who have
previously not purchased a Medicare supplement policy, those who have
not had a policy within the last 31 days or those who have lost or
been removed from group coverage within the preceding 63 days.
MEDICARE
SELECT POLICY: A policy or certificate that contains restricted
network provisions. This type of policy may require you to use hospitals
and in some cases, doctors within its network to be eligible for full
benefits.
SUPPLEMENTAL (Medigap Insurance) INSURANCE: You can buy supplemental coverage that pays
for some things original Medicare doesn’t cover, like deductibles,
doctor and hospital coinsurance and emergency care outside the country.
Private insurance companies offer this supplemental coverage, often
called “Medigap” insurance. You can sometimes continue
insurance coverage through a former employer.
Federal regulations
mandate that all Medicare supplemental policies offer the same set of
benefits. That’s why, when deciding what company to buy from,
the most important factors to consider are cost and stability. There
are 12 different Medicare supplement plans, labeled A-L (except in Massachusetts, Minnesota and Wisconsin) Plan A offers the fewest benefits
and is usually the least expensive.
Return to Top

|

 The
Qualified Medicare Beneficiary Program
The
Qualified Medicare Beneficiary Program Companies may not refuse to issue a
Companies may not refuse to issue a  Medicare covers physician services, outpatient hospital services,
lab services, X-ray, radiation and therapy services, home health visits,
physical therapy, speech pathology services, some forms of vaccinations,
durable medical equipment, limited ambulance services, prosthetic
devices, immunosuppressive drugs for the first year following an organ
transplant, and other medical supplies and equipment.
Medicare covers physician services, outpatient hospital services,
lab services, X-ray, radiation and therapy services, home health visits,
physical therapy, speech pathology services, some forms of vaccinations,
durable medical equipment, limited ambulance services, prosthetic
devices, immunosuppressive drugs for the first year following an organ
transplant, and other medical supplies and equipment. 
 Plan K:
Plan K:
